What is the best treatment for uterine fibroids?
The treatment of uterine fibroids depends on the size and location of the fibroid, as well as the severity of the symptoms: Medical treatment for mild cases relieves symptoms and slows growth, while laparoscopic myomectomy for advanced cases removes the fibroid while preserving the uterus and improving fertility. A hysterectomy is a definitive solution for severe cases.
🩺 Are you suffering from uterine fibroid symptoms?
The importance of discussing uterine fibroid treatment lies in the fact that this condition, despite being benign in most cases, can cause severe bleeding, chronic pain, menstrual irregularities, and in some instances, may even affect fertility and pregnancy.
Uterine fibroids are among the most common gynecological issues, affecting a large percentage of women of childbearing age. Some women may discover them by chance without experiencing any symptoms, while others suffer from health problems that significantly impact their daily lives.
What is a Uterine Fibroid?
A uterine fibroid is an abnormal growth of smooth muscle cells in the wall of the uterus. It is considered a benign tumor that does not spread to other parts of the body.
These tumors typically grow slowly and can appear as a single fibroid or multiple fibroids of varying sizes, ranging from very small growths invisible to the naked eye to large masses that can alter the shape of the uterus.
💡 Important Information
A fibroid is not cancer, but its location inside or around the uterus determines how much it impacts a woman's health. It usually grows under the influence of the estrogen hormone, which is why it appears during reproductive years and may shrink after menopause.
Causes of Uterine Fibroids
To date, there is no single definitive cause for the development of uterine fibroids, but medical research points to several contributing factors:
- Female Hormones: High levels of estrogen and progesterone can stimulate the growth of fibroid cells.
- Genetics: Women with a family history of fibroids are at a higher risk.
- Genetic Alterations: Changes that cause uterine cells to divide abnormally.
- Lifestyle: Weight gain and lack of physical activity (contributing factors).
Types of Uterine Fibroids Based on Location
Fibroids are classified into several types based on where they grow, which is a key factor in determining symptoms and the treatment approach:
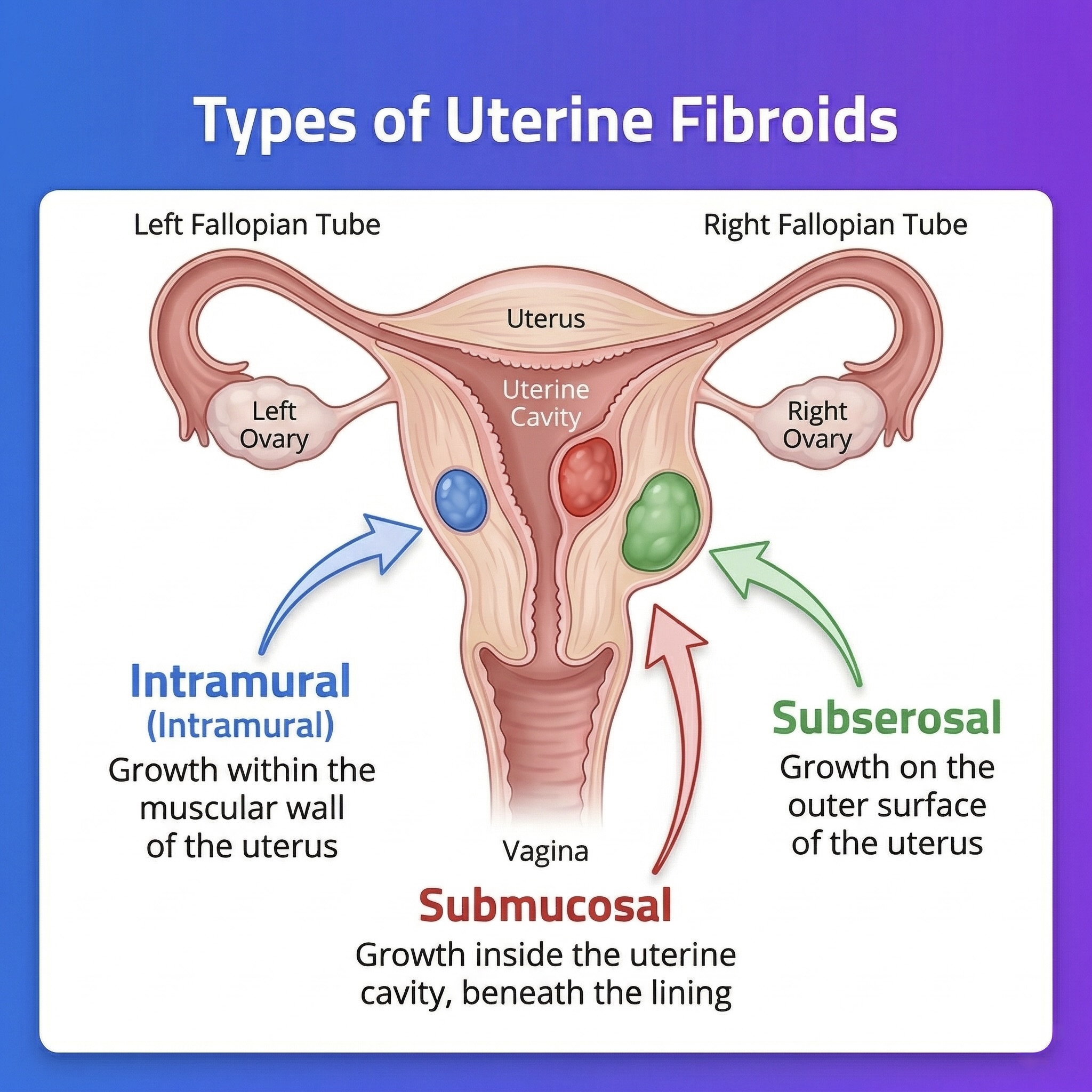
| Type | Location | Main Symptoms | Impact on Fertility |
|---|---|---|---|
| Intramural | Within the uterine muscle wall | Uterine enlargement, heavy bleeding | Moderate |
| Submucosal | Inside the uterine cavity | Heavy and irregular bleeding | High ⚠️ |
| Subserosal | On the outer surface of the uterus | Pressure on the bladder/bowel | Low |
Fibroid Sizes and Complications
The impact of a fibroid is not limited to its type and location; its size plays a major role in the manifestation of symptoms:
- Small Fibroids (less than 3 cm): May not cause any issues and can remain undetected for years.
- Medium Fibroids (3-5 cm): May cause mild bleeding and pain.
- Large Fibroids (larger than 5 cm): Noticeable abdominal enlargement, continuous pelvic pressure, and heavy bleeding that can lead to anemia.
⚠️ Complications of Large Fibroids
The larger the fibroid, the higher the likelihood of developing anemia, chronic fatigue, and distortion of the uterine cavity, which can hinder pregnancy.
Symptoms of Uterine Fibroids
Symptoms vary from one woman to another and depend on the size, location, and number of fibroids:
Common Symptoms
- Heavy bleeding during menstruation, often with blood clots.
- Pelvic pain or lower abdominal pain radiating to the back.
- A feeling of pressure or fullness in the abdomen.
- Frequent urination due to pressure on the bladder.
- Constipation due to pressure on the bowels.
- Pain during sexual intercourse.
- Delayed pregnancy or difficulty conceiving.
⚠️ Complications of Recurrent Bleeding
Recurrent heavy bleeding can lead to anemia, chronic feelings of fatigue and exhaustion, shortness of breath, and dizziness.
When Do Uterine Fibroids Become Dangerous?
In most cases, uterine fibroids are benign and do not pose a direct threat. However, they become a source of concern when:
- They cause severe bleeding leading to acute anemia.
- They grow rapidly and abnormally.
- They compress adjacent organs (bladder, ureters, intestines).
- They cause fertility issues or distort the uterine cavity.
How are Uterine Fibroids Diagnosed?
Diagnosis begins with a medical history and pelvic exam, followed by imaging tests:
- Ultrasound: The most common method used to determine the number, sizes, and locations of fibroids.
- MRI (Magnetic Resonance Imaging): For a more detailed image when planning for surgery.
- Hysteroscopy: To examine the inside of the uterine cavity.
Treatment of Uterine Fibroids
The choice of treatment for uterine fibroids is based on the woman's age, symptom severity, fibroid size and location, and her desire for future pregnancy:
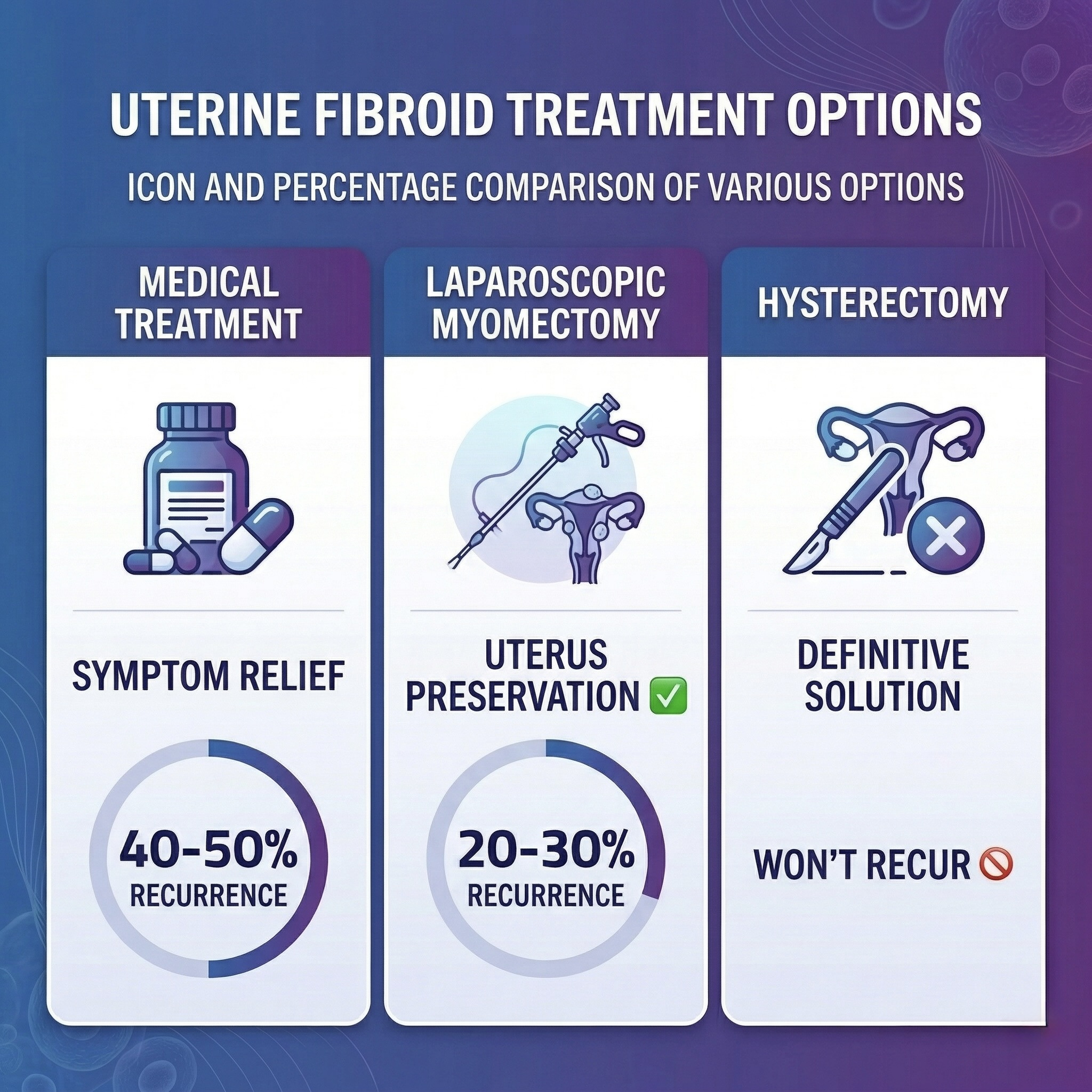
Comprehensive Comparison: Medical vs. Surgical Treatment
| Criteria | Medical Treatment | Laparoscopic Myomectomy | Hysterectomy |
|---|---|---|---|
| Suitable Candidates | Mild to moderate symptoms | Women desiring pregnancy | Severe multiple fibroids |
| Objective | Symptom relief | Remove fibroid + preserve uterus | Definitive solution |
| Fertility Preservation | Yes | Yes | ❌ No |
| Recurrence Rate | High (40-50%) | Moderate (20-30%) | Will not recur |
| Recovery Time | — | 1-2 Weeks | 4-6 Weeks |
Non-Surgical Treatment of Uterine Fibroids
The goal is to control symptoms, reduce bleeding, and slow tumor growth by affecting hormonal balance. This is suitable for mild cases or women approaching menopause.
💡 Note
Medical treatment does not completely remove the fibroid, but rather aims to manage its impact. It requires regular medical follow-up.
When is Non-Surgical Treatment Not Enough?
Despite the effectiveness of conservative treatment, it may not be suitable in the following situations:
- Severe bleeding leading to acute anemia.
- The fibroid is large and compressing adjacent organs.
- There is a clear impact on fertility.
- Lack of response to medications or a return of symptoms after improvement.
Surgical Treatment of Uterine Fibroids
Surgical treatment is a primary solution when symptoms are severe or conservative treatment fails:
Myomectomy (Fibroid Removal Preserving the Uterus)
Suitable for women wishing to conceive. It is performed via Laparoscopy (most common) or open surgery.
Hysterectomy as a Definitive Treatment
The most effective solution for women who do not wish to have children in the future, or when there are large and multiple fibroids.
Do Fibroids Return After Treatment?
Hysterectomy: The fibroid will not return. Myomectomy (Removal of fibroid only): There is a chance of new fibroids forming (20-30%). Medical Treatment: They may grow back when medication is stopped.
🎬 Watch: Explanatory Video About Uterine Fibroids
📚 Related Articles
Impact of Fibroids on Pregnancy and Fertility
The impact of fibroids on pregnancy varies depending on their size and location. In some cases, they don't interfere at all, while in others they may cause:
- Prevention of egg implantation if located inside the uterine cavity.
- Distortion of the uterine shape, which can obstruct sperm movement.
- Increased risk of miscarriage in the first trimester.
- Premature birth or bleeding.
💡 Good News
Many women with uterine fibroids have normal pregnancies and deliveries, especially if the fibroid is small and does not affect the uterine cavity.
Are you suffering from fibroid symptoms?
Book your consultation now with Dr. Mohamed El-Senity - Expert in Gynecological Laparoscopic Surgeries

Prof. Dr. Mohamed Abdel Fattah El-Senity
Consultant Obstetrician and Gynecologist
Expert in Gynecological Laparoscopic Surgeries
Ain Shams University Hospitals
+20 Years ExperienceFrequently Asked Questions About Uterine Fibroid Treatment
📚 Scientific Sources
- Mayo Clinic - Uterine Fibroids
- ACOG - Management of Uterine Fibroids 2024
- NIH - Fibroid Treatment Guidelines
- WHO - Women's Health Statistics
⚕️ Medical Disclaimer
This content is for health education purposes only and is not a substitute for professional medical advice. Every case is different and must be evaluated individually.
