Endometriosis Treatment: The Complete Guide 2026
What is the best treatment for endometriosis?
Endometriosis treatment depends on the severity and stage of the condition: Medical (hormonal) treatment for mild to moderate cases reduces pain and slows disease progression, while laparoscopic surgical treatment for advanced cases removes disease foci and improves fertility by up to 50–70%. Combined therapy integrating medication and surgery yields the best outcomes.
What is Endometriosis?
Endometriosis is a medical condition in which tissue similar to the uterine lining grows outside the uterine cavity — in places it shouldn't exist, such as the ovaries, fallopian tubes, the pelvic cavity, and sometimes the intestines or bladder.
This tissue responds to monthly hormonal changes just like the normal uterine lining — it thickens and bleeds with each menstrual cycle, but has no way to exit the body, leading to chronic inflammation, adhesions, scar tissue, and blood-filled cysts known as chocolate cysts (endometriomas).
Important Warning
In its advanced stages, endometriosis can cause ureter obstruction and complete renal failure. The disease may not appear on a regular ultrasound and may require diagnostic laparoscopy.
Stages of Endometriosis
Endometriosis is classified into four main stages based on the extent and depth of the migrated tissue and its effect on surrounding organs:
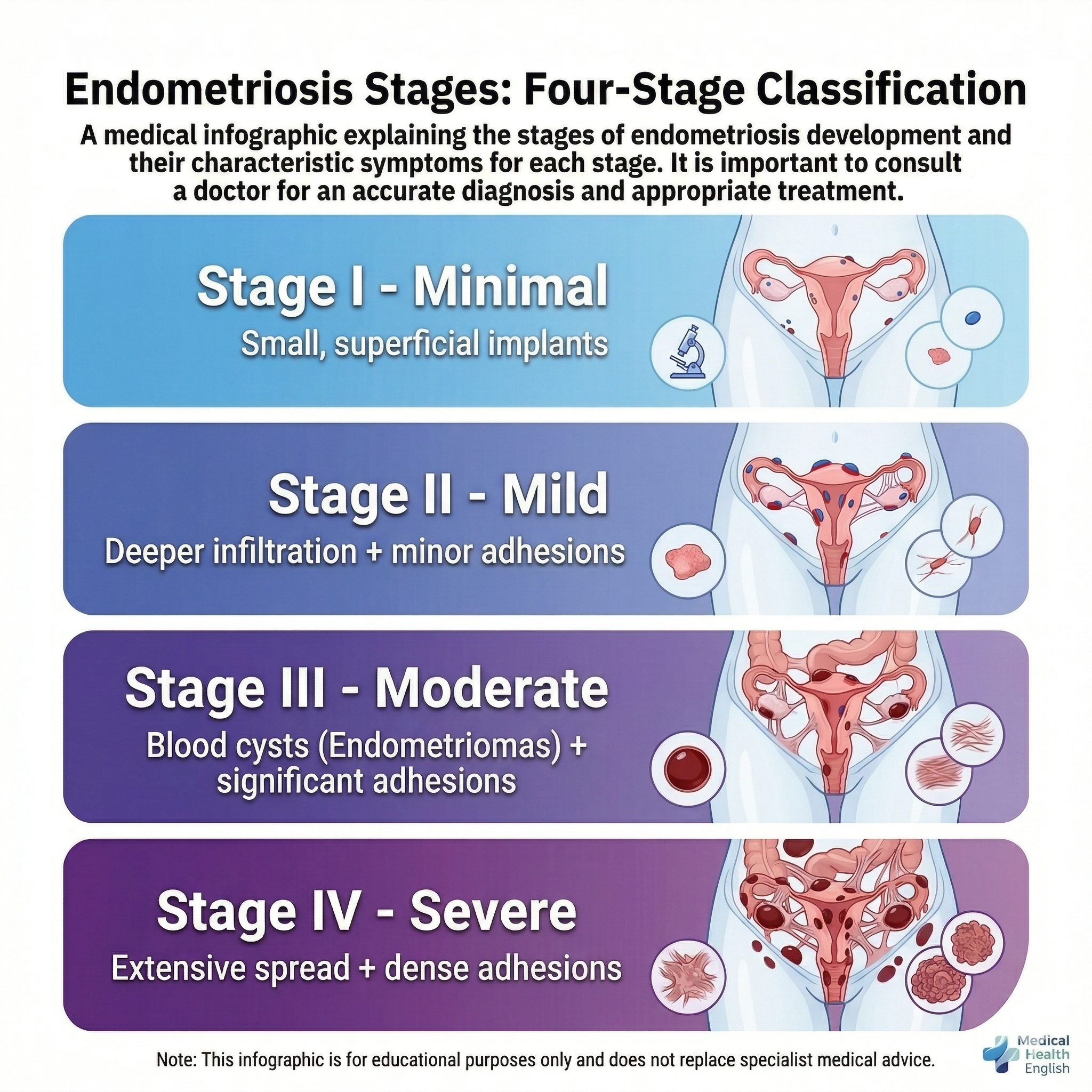
| Stage | Description | Symptoms | Appropriate Treatment |
|---|---|---|---|
| Stage I (Minimal) | Small, superficial foci | May not cause severe symptoms | Medical treatment |
| Stage II (Mild) | Deeper penetration + minor adhesions | Menstrual pain | Medical or surgical treatment |
| Stage III (Moderate) | Blood-filled cysts + visible adhesions | Severe pain and fertility problems | Surgical treatment via laparoscopy |
| Stage IV (Severe) | Wide spread + dense adhesions | Severe pain affecting organs | Advanced surgery via laparoscopy |
Causes of Endometriosis
To date, there is no single confirmed cause of endometriosis, but several medical theories exist:
- Retrograde Menstruation Theory: a portion of menstrual blood flows back through the fallopian tubes into the pelvic cavity, carrying uterine lining cells
- Genetic Factors: increased likelihood if there is a family history of the disease
- Immune System Disorders: may prevent the body from eliminating abnormal cells
- Elevated Estrogen Levels: may stimulate tissue growth outside the uterus
Symptoms of Endometriosis
Symptoms vary from woman to woman. They typically appear two weeks or 10 days before the menstrual period and continue throughout it:
Common Symptoms
- Chronic pelvic pain that worsens during menstruation
- Severe menstrual cramps that do not respond to standard pain relief
- Pain during or after intercourse
- Digestive issues such as bloating, constipation, or diarrhea
- Heavy bleeding or prolonged menstrual periods
- Delayed pregnancy or difficulty conceiving
Unusual Symptoms
- Nasal bleeding
- Blood in urine or with coughing
- Abdominal bloating and general fatigue
- Muscle pain and back pain
How is Endometriosis Diagnosed?
Diagnosing endometriosis can be challenging, as its symptoms overlap with many other gynecological disorders:
- Medical history: nature of pain, timing, and its relation to the cycle
- Physical examination: to detect masses or tender areas
- Ultrasound: may reveal blood-filled cysts on the ovaries
- MRI: to precisely assess disease extent
- Diagnostic laparoscopy: the definitive diagnosis and simultaneously a treatment option
Endometriosis Treatment
Endometriosis treatment depends on symptom severity, disease stage, patient age, and desire for pregnancy:
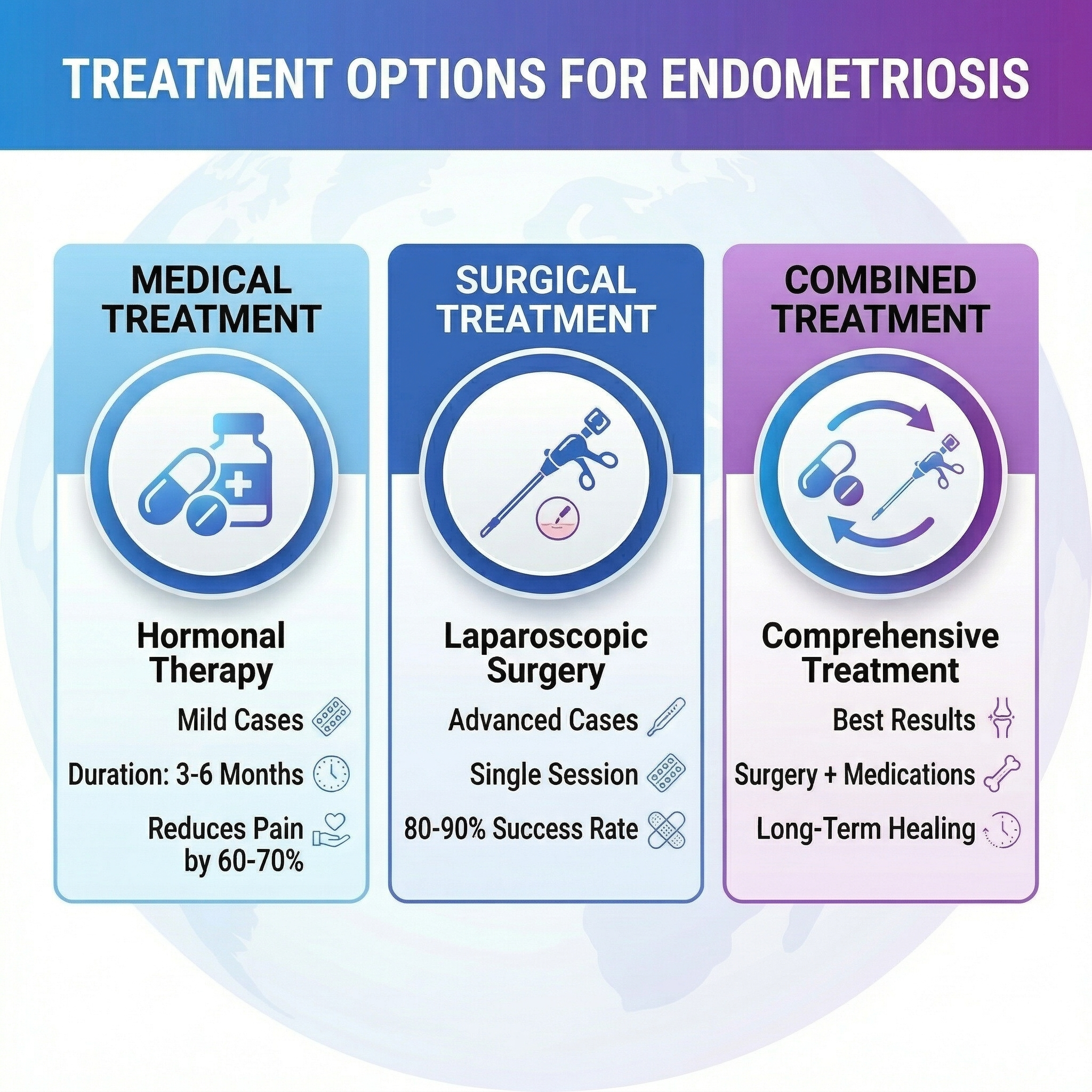
Full Comparison: Medical vs. Surgical Treatment
| Criterion | Medical Treatment | Laparoscopic Surgery |
|---|---|---|
| Suitable Cases | Stages I and II | Stages III and IV |
| Treatment Duration | 3–6 months continuous | One session (1–3 hours) |
| Pain Improvement Rate | 60–70% | 80–90% |
| Fertility Improvement | ❌ Very Limited | ✅ 50–70% |
| Disease Recurrence | 40–50% | 20–30% |
| Side Effects | Hot flashes, mood changes | Anesthesia risks (rare) |
| Cost | Lower cost | Higher but lasting results |
Medical Treatment (Non-Surgical)
Aims to reduce pain, limit the activity of migrated tissue, and slow disease progression by regulating hormonal changes in the body.
Important Note
Medical treatment does not improve fertility or conception chances, but surgical treatment significantly helps with recovery and pregnancy.
Laparoscopic Surgical Treatment
Recommended in cases that do not respond to conservative treatment or when symptoms are severe. The goal is to remove as much migrated tissue as possible and break down adhesions.
- Excision or ablation of disease foci
- Removal of blood-filled cysts (endometriomas)
- Breaking down adhesions while preserving healthy organs
- Minimally invasive technique that reduces pain and speeds recovery
Related Articles from Our Website
Watch: Quick Explanation of Endometriosis
Does Endometriosis Return After Removal?
Disease recurrence can occur after surgery at a rate of 25–35%. Main causes of recurrence:
- Delaying treatment until the cyst reaches 5–7 cm before surgery
- Incorrect use of medical treatment before surgery
- Improper surgical technique — incomplete cyst removal
- Removing a large cyst in a single surgery instead of staged procedures
Impact of Endometriosis on Pregnancy and Fertility
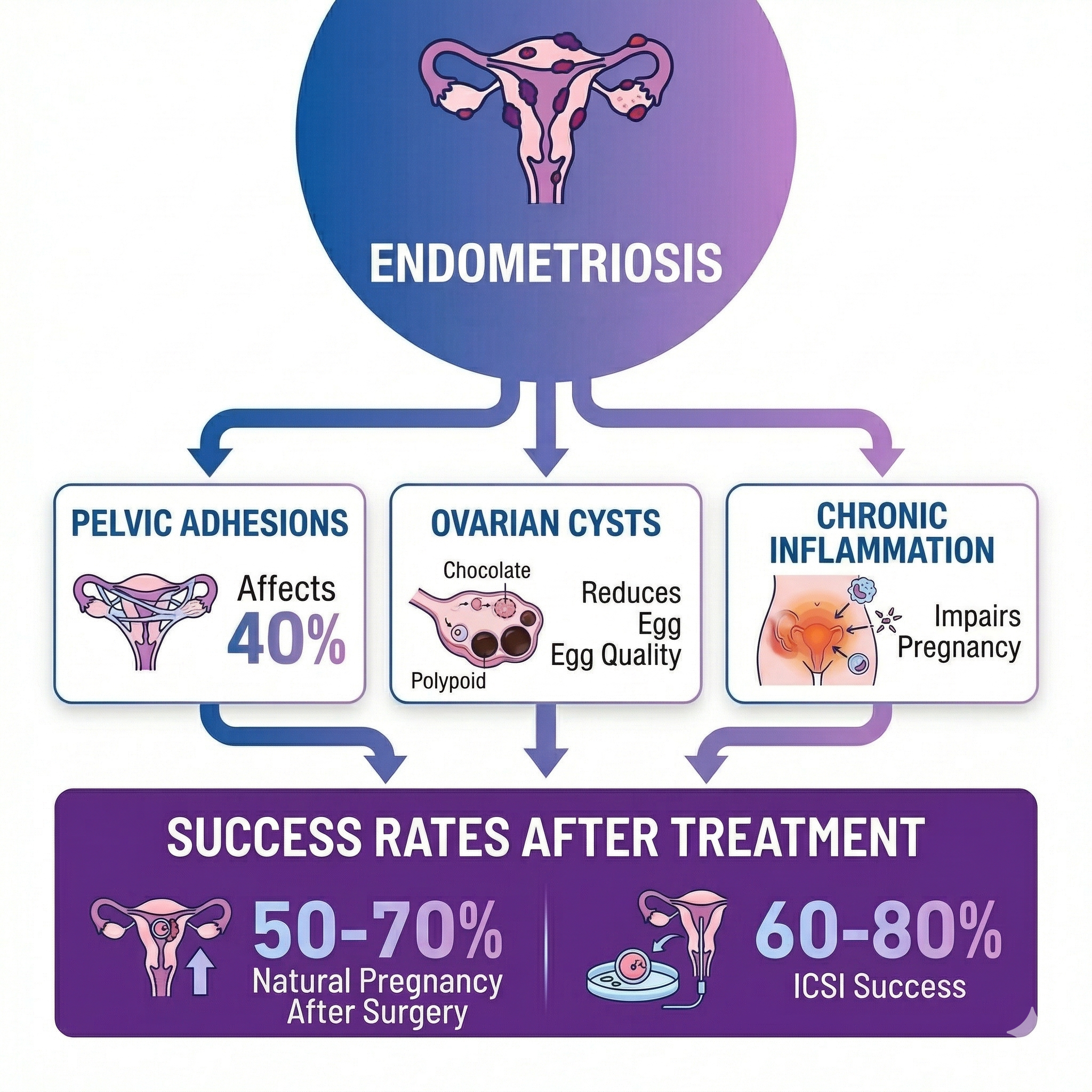
Endometriosis affects fertility in several ways:
- Adhesions: obstruct egg movement or sperm access
- Blood-filled cysts: impair ovarian function and egg quality
- Chronic inflammation: alters the environment needed for conception
Good News!
After surgical treatment, fertility improves by 50–70% in a large number of women. IVF success rates reach 60–80%.
When Should You See a Doctor Immediately?
Signs That Require Immediate Evaluation
Persistent pelvic pain over extended periods, heavy or irregular bleeding, pain accompanied by vomiting or dizziness, difficulty conceiving without an obvious cause. Early diagnosis preserves fertility and prevents complications.
Are You Experiencing Endometriosis Symptoms?
Book your consultation now with Dr. Mohamed El-Senity – Expert in Gynecological Laparoscopy
Book Your Appointment Now
Prof. Dr. Mohamed Abd El-Fattah El-Senity
Expert in Gynecological Laparoscopy
❓ Frequently Asked Questions About Endometriosis Treatment
Scientific Sources
- Mayo Clinic – Endometriosis Diagnosis and Treatment
- National Institutes of Health (NIH) – Medical Management of Endometriosis 2024
- World Health Organization (WHO) – Endometriosis Fact Sheet
- American College of Obstetricians and Gynecologists (ACOG) – Endometriosis Guidelines
Medical Disclaimer: The information in this article is for educational purposes only and does not replace consultation with a specialist. Please see a qualified physician for diagnosis and appropriate treatment.
